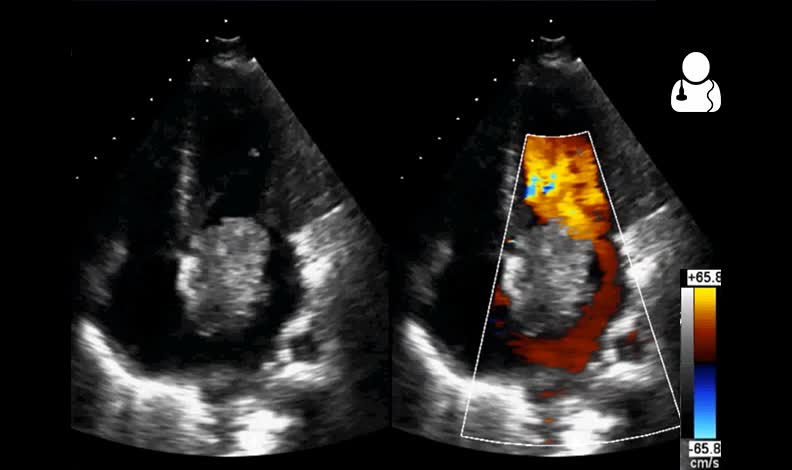
The patient is an 11 year old male who was leaving soccer practice when his family witnessed him suddenly collapse. He was then noted to have left sided hemiparesis associated with a headache and nausea/vomiting, and was airlifted to your emergency department. Noncontrast CT of the brain was negative, but CTA revealed a complete proximal right M1 occlusion. You perform a bedside echocardiogram:

Answer: Atrial Myxoma
This bedside echo reveals a large pedunculated left atrial mass that appears to prolapse into the left ventricle during diastole. This mass causes subtotal occlusion of the mitral inflow tract when it prolapses. LV systolic function appears to be well maintained with a visually normal ejection fraction.
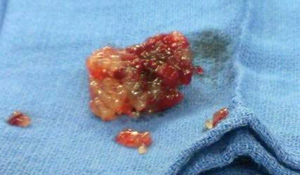 This patient was taken to angiography by neurosurgery and underwent an interventional embolectomy. A fatty, “grape-cluster” appearing mass was recovered (picture, right). Following the embolectomy, the patient was taken to the PICU where he was already showing signs of improved left sided strength. Subsequently, the patient was referred to cardiothoracic surgery for the atrial mass, which was successfully resected and confirmed to be an atrial myxoma. The final clinical outcome was 4/5 left sided strength and no recurrent CVAs.1
This patient was taken to angiography by neurosurgery and underwent an interventional embolectomy. A fatty, “grape-cluster” appearing mass was recovered (picture, right). Following the embolectomy, the patient was taken to the PICU where he was already showing signs of improved left sided strength. Subsequently, the patient was referred to cardiothoracic surgery for the atrial mass, which was successfully resected and confirmed to be an atrial myxoma. The final clinical outcome was 4/5 left sided strength and no recurrent CVAs.1
- Pediatric strokes are typically not due to the atherosclerotic disease that so commonly plagues adults. A cardiac etiology has been implicated in 19% of cases in the Canadian Pediatric Stroke Registry.2
- This case illustrates how a myxoma may fragment and embolize, causing ischemic stroke. It is unlikely that this patient would have responded to IV thrombolytics; interventional treatment should be considered in cases of CVA with cardiac mass.
- Rhabdomyoma is the most common pediatric cardiac mass, but atrial myxoma is more likely to result in thromboembolism due to its pedunculated and friable nature.1 In one study 21% of patients with an atrial myxoma suffered embolic CVA.
- Common cardiac manifestations of atrial myxoma include heart failure and syncope.3
- In adults, TTE has been shown to be 93% sensitive for cardiac tumors, while TEE increases the sensitivity to 96.8%.4
Case submitted by Scott Sparks, MD
@EDsparkyur
- Thom CD, Sparks SE. Acute pediatric stroke-what’s the hurry? A case for emergency physician-performed echocardiography. Am J Emerg Med. 2014;32:(11)1440.e3-5. [pubmed]
- Roach ES, deVeber G, Riela AR, Wiznitzer M. Recognition and Treatment of Stroke in Children. National Institute of Neurologic Disorders and Stroke (http://www.ninds.nih.gov/). Accessed December, 2014. [article]
- Ekinci EI, Donnan GA. Neurological manifestations of cardiac myxoma: a review of the literature and report of cases. Intern Med J. 2004;34:(5)243-9. [pubmed]
- Meng Q, Lai H, Lima J, Tong W, Qian Y, Lai S. Echocardiographic and pathologic characteristics of primary cardiac tumors: a study of 149 cases. Int J Cardiol. 2002;84:(1)69-75. [pubmed]