The patient is a 39 y/o female with a h/o lupus who is post-op day #7 status-post renal transplant. The patient complains of abdominal pain with gross hematuria for several days. Upon arrival, the patient’s initial vitals were a BP of 137/59 and a pulse of 91. Examination showed cold extremities, moderate diffuse abdominal tenderness/distension and a pale tongue.
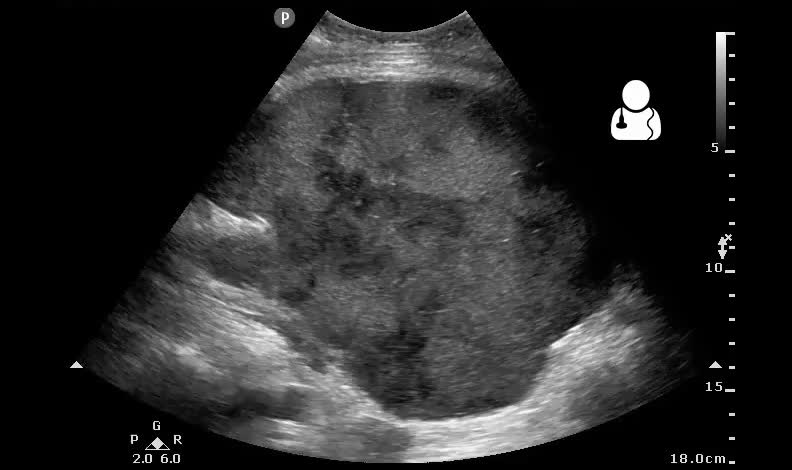
I-stat hematocrit was noted to be 5, and so the patient was given 4 units of pRBCs and surgery was consulted. Suddenly the patient becomes unresponsive in front of you, and you are unable to palpate any pulses. Standard ACLS was followed and the patient obtained ROSC. Repeat abdominal scan showed the following.

Diagnosis: large post-op hematoma and hemorrhage
In the OR, they removed a large amount of clot and old hemorrhage. There was s a small laceration seen at the posterior portion of the transplant renal parenchyma. There was some communication of old blood from the intra-abdominal portion into the retroperitoneum via the ovarian ligaments.
- The most common surgical complications involving renal transplants are renal vein thrombosis, renal artery thrombosis,
 ureter obstruction, urine leak and a wound infection.1
ureter obstruction, urine leak and a wound infection.1 - Bleeding is uncommon after a surgery, and if it does occur, is usually due to unligated vessels in the graft hilum or from small severed retroperitoneal vessels of the recipient.1 In this patient, it was from a laceration to the donor kidney.
- Risk factors for post-surgical bleeding include recipient obesity, antiplatelet agents, and anticoagulation.1
- Abdominal ultrasound has been found to reliably detect between 250-620 mL of intraperitoneal fluid.2
- Humar A, Matas AJ. Surgical complications after kidney transplantation. Semin Dial. 2005;18(6):505-10.
- Rose J. Ultrasound in Abdominal Trauma. Emerg Med Clin N Am 2004;22:581-99