A 65 year old male presents to emergency department with a one week history of nausea and lethargy. He reports having consulted his GP early into his symptoms, for which he was given a course of antibiotics. He reports that his symptoms have not improved. The emergency physician sends blood work and the patient’s creatinine comes back at 18mg/dl with urea of 42mmol/L and K of 6.8. Patient is referred to Critical care for urgent dialysis. On further probing by the critical care team, patient reports history of occasional chills over the past one week and has also noticed that his urine output may have been lower than normal. The critical care physician places a probe on the patient’s abdomen and this is what he sees:

Answer and pearl: Obstructive uropathy
- Obstructive uropathy accounts for about 10% of the cases of Acute kidney injury and 4% of cases of chronic renal failure. Stone disease is one of the most common causes of obstruction. Other causes include malignancy, inflammatory (tuberculosis, schitsosomiasis, amyloidosis, endometriosis ) and congenital (ureteric stricuture, renal cyst, ureterocoele).1
- Obstructive uropathy is responsible for a wide range of metabolic and electrolyte abnormalities that may lead to renal failure especially if the obstruction is bilateral. Patients may not be aware or have only mild symptoms if the progress is gradual and may present in frank renal failure
- Ultrasonography, CT and CT urography are the gold standard diagnostic tests. US is often the first imaging performed.2
- The hallmark of obstruction on US is the presence of hydronephrosis. Prominent anechoic structures in the renal sinus represent a dilated pelvi-calyceal system and calculi may be demonstrated as echogenic focus with or without shadowing.
- The degree of hydronephrosis can be estimated visually:
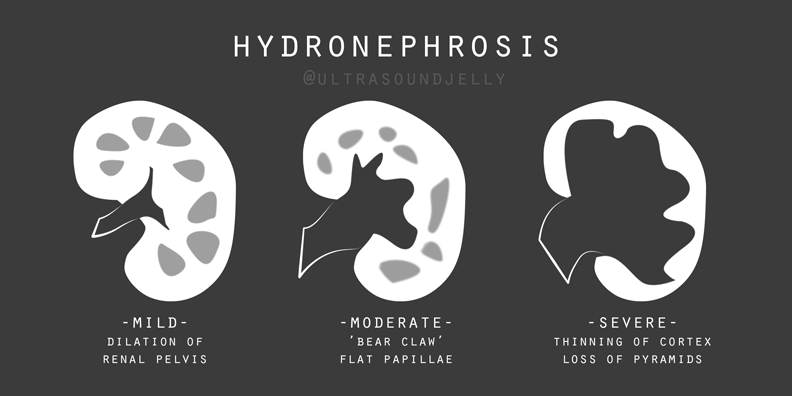
Limitations of US:
- The false negative rate with US is as high as 35% in patients with ureteric calculus. Technical limitations such as bowel gas, obesity can hamper imaging.
References





