A 59-year old female presented to a community hospital with subjective shortness of breath that has been worsening over the past few days. She denies chest pain, nausea and vomiting or fever. Vital signs are as follows: HR 142, BP 114/89, RR 20, temp 98.7°F (37°C). Physical exam demonstrates tachycardia and equal bilateral normal breath sounds. Bedside ultrasound is performed at the bedside and the following images are obtained:
What do the images show? What is the diagnosis? (Click the button for the answer!)

Pericardial effusion with RV collapse; lack of respirophasic variation of IVC indicative of pericardial tamponade
On a review of the patients electronic medical record, she had a pacemaker placed a few months ago, but had only had shortness of breath symptoms over the past few days. POCUS images were shared with a cardiologist at a tertiary hospital who agreed with the findings. The patient was subsequently transferred and had a successful pericardial drainage in the cath lab.
Beck’s triad, which is “falling arterial pressure, rising venous pressure and small quiet heart” is often quoted as required for the clinical diagnosis of tamponade. However, the initial publication (published in 1935) is based on a case report of 2 patients.1 In fact, the majority of the patients with proven tamponade are hypertensive or normotensive. 2
The most specific sonographic finding of sonographic tamponade is right ventricular diastolic collapse. Once pericardial pressures exceed the diastolic pressure in the RV, obstructive shock is likely to be present as the RV is no longer able to fill.3 However in our patient it was difficult to identify if the RV collapse was happening in diastole or systole. In the 4th ultrasound clip, the IVC is visualized. If the IVC is seen to have minimal respirophasic variation (change in diameter with respiration), the patient is very likely to have an elevated CVP, which is consistent with obstructive shock (i.e., pericardial tamponade).4
Pearls:
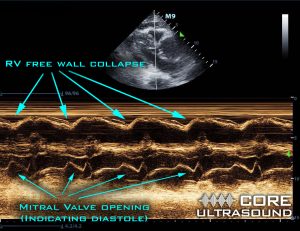
- To help identify if the RV is collapsing during diastole or systole, hit the freeze button and scroll to where the mitral valve is open, representing diastole.
- Alternatively, the high frame rate of M-mode can be used to determine diastolic collapse. This is done by placing the cursor through the RV free wall and mitral valve in the parasternal long axis. If RV collapse occurs when the mitral valve is open, this is indicative of RV diastolic collapse.
- Besides IVC dilation and RV collapse, RA collapse, MV and TV inflow variation can be helpful in the diagnosis of pericardial tamponade.4
- Hypertension may actually be more common than recognized in the presentation of subacute tamponade patients. One review found 27-43% of patients presented with a SBP >120mmHg and had confirmed tamponade by cath lab. Absence of hypotension does not necessarily indicate the patient is not critically ill. 5
Click here for the full case!
Case Courtesy of Lindsay Reardon, MD
Case Written by Jacob Avila, MD
Peer Reviewed by Terren Trott, MD
References
- Roy CL, Minor MA, Brookhart MA, Choudhry NK. Does this patient with a pericardial effusion have cardiac tamponade?. JAMA. 2007;297(16):1810-8.
- Kapoor T, Locurto M, Farina GA, Silverman R. Hypotension is Uncommon in Patients Presenting to the Emergency Department with Non-traumatic Cardiac Tamponade The Journal of Emergency Medicine. 2012; 42(2):220-226.
- Argulian E, Messerli F. Misconceptions and facts about pericardial effusion and tamponade. Am J Med. 2013;126(10):858‐861. doi:10.1016/j.amjmed.2013.03.022
- Himelman RB, Kircher B, Rockey DC, Schiller NB. Inferior vena cava plethora with blunted respiratory response: a sensitive echocardiographic sign of cardiac tamponade. J Am Coll Cardiol. 1988;12(6):1470‐1477. doi:10.1016/s0735-1097(88)80011-1
- Argulian E, Herzog E, Halpern DG, Messerli FH. Paradoxical hypertension with cardiac tamponade. Am J Cardiol. 2012;110(7):1066‐1069. doi:10.1016/j.amjcard.2012.05.042



