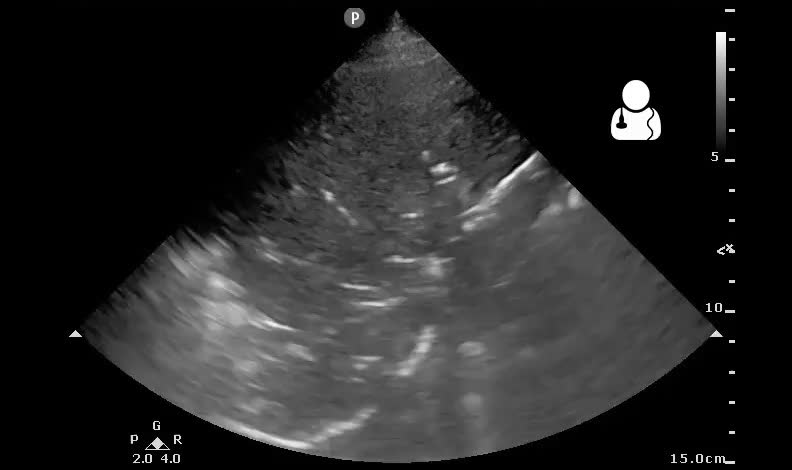
67 yo nursing home patient presents with altered mental status. Vitals signs are as follows: BP 92/78, HR: 115, RR: 35, O2 sat: 89%. Patient is moaning and uncooperative with the physical exam. On auscultation, you are unable to appreciate any overt lobular rales or wheezing. You think you feel a distended bladder in the suprapubic region. Ultrasound shows the following in the right posterior lung field. What is the finding and diagnosis?

Diagnosis: Pneumonia
Placing the probe on the right posterolateral lung field, you see something abnormal. Instead of seeing a linear pleural line between ribs and a-lines, you see a hypoechoic pulmonary consolidation that contains hyperechoic lines and flecks that move with respiration. These are known as air bronchograms.
- Typically, the diagnosis of pneumonia is performed based off of the patients’ clinical exam, history, labs and x-ray. However, these tests have been shown to be unreliable and inaccurate.
- A JAMA meta analysis concluded that no individual or combined clinical findings have been found to accurately predict whether or not a patient has pneumonia.1
- X-ray has been found to have a sensitivity ranging from 46-77% when a CT scan is used as the gold standard. Those same studies show US to have a sensitivity ranging from 93-100%.2-7
- Two meta-analyses evaluating ultrasound in the diagnosis of pneumonia were published in 2014, one of which included 9 studies and found US to have a +LR of 15.6 and a –LR of 0.03.8 The other included 10 studies and found a +LR of 16.8 and a –LR of 0.07.9
- Multiple signs have been described to facilitate the diagnosis of pneumonia on ultrasound, including air bronchograms, b-lines, subpleural consolidations, pleural line abnormalities, pleural effusions and fluid bronchograms.
- The most specific sign for the diagnosis of pneumonia is the presence of air bronchograms, which are hyperechoic lines and dots within a hypoechoic area, thought to represent air trapped in small airways within a consolidation.10
- Air bronchograms are divided into two types: Dynamic and Static.
- If the bronchograms are mobile, they are considered dynamic air bronchograms and are thought to be pathognomonic for pneumonia. If the bronchograms are immobile they are then called static air bronchograms which can be seen in both atelectasis and pneumonia.5 Here is an example of static and dynamic air bronchograms next to each other:
- Metlay JP, Kapoor WN, Fine MJ. Does this patient have community-acquired pneumonia? Diagnosing pneumonia by history and physical examination. JAMA 1997;278:1440–5. [pubmed]
- Xirouchaki N, Magkanas E, Vaporidi K, et al. Lung ultrasound in critically ill patients: comparison with bedside chest radiography. Intensive Care Med. 2011;37(9):1488-93. [pubmed]
- Bourcier JE, Paquet J, Seinger M, et al. Performance comparison of lung ultrasound and chest x-ray for the diagnosis of pneumonia in the ED. Am J Emerg Med. 2014;32(2):115-8. [pubmed]
- Cortellaro F, Colombo S, Coen D, Duca PG. Lung ultrasound is an accurate diagnostic tool for the diagnosis of pneumonia in the emergency department. Emerg Med J. 2012;29(1):19-23. [pubmed]
- Parlamento S, Copetti R, DiBartolomeo S. Evaluation of lung ultrasound for the diagnosis of pneumonia in the ED. Am J Emerg Med. 2009;27:379-84. [pubmed]
- Reissig A, Copetti R, Mathis G, Mempel C, Schuler A, Zechner P et al. Lung Ultrasound in the Diagnosis and Follow-up of Community-Acquired Pneumonia. Chest. 2012;142:965–972. [pubmed]
- Liu XL, Lian R, Tao YK, Gu CD, Zhang GQ. Lung ultrasonography: an effective way to diagnose community-acquired pneumonia. Emerg Med J. 2014. [pubmed]
- Hu QJ, Shen YC, Jia LQ, et al. Diagnostic performance of lung ultrasound in the diagnosis of pneumonia: a bivariate meta-analysis. Int J Clin Exp Med. 2014;7(1):115-21. [pubmed]
- Chavez MA, Shams N, Ellington LE, et al. Lung ultrasound for the diagnosis of pneumonia in adults: a systematic review and meta-analysis. Respir Res. 2014;15:50. [pubmed]
- Weinberg B, Diakoumakis EE, Kass EG, Seife B, Zyi ZB. The air bronchogram: Sonographic demonstration. AJR Am J Roentgenol. 1986;147:593-5. [pubmed]